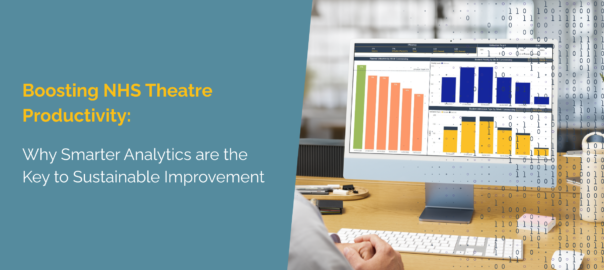
30-minute video
Speakers:
Andrena Weston, Divisional Director of Operations, The Shrewsbury and Telford Hospital NHS Trust
Siân Webley, Divisional Director of Operations, Walsall Healthcare NHS Trust
Transcript
23 October 2025, 12:30pm
Stephen Dorrell
Good afternoon to everyone. My name is Stephen Dorrell. Those with a very, very long memory may remember me from long ago as a health minister and I have been around for the health field ever since.
For this purpose, I am a director engaged with Four Eyes Insight and it’s a great pleasure to welcome you to this webinar, where we’re looking at an area of particular importance to Four Eyes certainly, but also to the health service and those who depend upon it. And that’s the question of outpatient productivity and how we can ensure that when we secure improvement in productivity in outpatients, those improvements endure and continue to the benefit both of patients and of taxpayers.
I’m going to offer a couple of thoughts before we start the webinar and then I’m going to introduce two people who know much more about it than I do. Indeed, will have forgotten more about it than I will ever know. But the thought of the importance of outpatients was very much the core of the NHS Confederation earlier this year when Jim Mackie famously said what we need to do is tear up the outpatient model.
I think everybody who cares about the health service that the outpatient model that we inherited is one that needs to be rethought, partly in order to deliver outpatient services more and more extensively in the community as one of the government’s clear objectives, partly in order to deliver outpatient services more efficiently so that that we can keep the finance director happy, but most importantly so that we respect the patients who rely on outpatient services and who find too often that the services don’t work in the way that they would want and we would want. So tear up the outpatient model and do it again, build it different, build it better is what we were challenged to do by Jim Mackey earlier this year and essentially that’s the theme that we are going to try to follow through.
In this webinar, how to do it and most importantly, once you’ve done it, how to make certain that those benefits continue to endure. Now I said we’ve got two people on the webinar who who do this day by day and one expert from Four Eyes in the form of Sam Sullivan, who’s director responsible for these services in Four Eyes.
But I’m going to ask first before going to Sam, I’m going to ask Siân Webley and Andrena Weston to introduce themselves. So Siân, first, why don’t you introduce yourself as the expert we know you to be in these services?
Siân Webley (WALSALL HEALTHCARE NHS TRUST)
Thank you, Stephen. Hi, everyone. My name’s Sian. I’m the Divisional Director of Operations here at Walsall Healthcare NHS Trust and my portfolio covers outpatients and elective care on behalf of the Trust.
Stephen Dorrell
OK. Thank you. And Andrena, please.
Andrena Weston (THE SHREWSBURY AND TELFORD HOSPITAL NHS TRUST)
Hello, I’m Andreena Weston. I’m acting divisional director of operations at Shrewsbury and Telford Hospital Trust. Within my portfolio sits outpatients and theatres and everything elective care. Thank you.
Stephen Dorrell
Fantastic. And so Sam, Samantha is very formal. I don’t think I’ve ever introduced you as Samantha, but Sam Sullivan, Delivery Director at Four Eyes, you’re going to lead us through this webinar.
Samantha Sullivan
Yeah, afternoon everyone. So I mean everything that Stephen said there, I’m sure it doesn’t come as a surprise to you. Outpatients is high on the agenda this this year. It’s where the patients sit, so the big risks sit in outpatients before people are in for their first appointment.
The general mass of patients, it’s an outpatient. So it’s one of the areas we’ve really got to get on top of and what we’re going to talk through today is the importance of setting the firm foundations. So how do we get the basics right that gives us the ability to build more innovative structures and transformational changes in outpatients. One of the key things that I think is important is how do we sustain that change once it’s actually been made.
So we’ve worked with Sian and Andrena on very similar projects over the last few years and what they’re going to talk through is what they’ve actually done since the projects have finished and how they’ve managed to sustain and continue to grow the improvements they’ve made in outpatients.
Before we get into any of the detail, we’re just going to do a quick poll just to understand what you feel your key challenges are in outpatients.
Poll:
What’s your biggest challenge in outpatients?
- Competing priorities
- Sheer scale of outpatients
- Data quality
- Demand growth/lack of resource and capacity
- Sustaining results
Here we go. So you you’ll either see a poll that’s just jumped onto your screen or will be in your chats. If you can just submit your answer and close the poll and we’ll come back to that in a few minutes time.
I just want to give you a bit of an overview about the work that we did with these two projects and then I’ll hand over to some Q&A with the with the panel. So just in terms of how the projects are structured, then it’s generally a 20 week project starts with a deep dive insight and discovery phase and then moves through into implementation.
Now these particular projects were all about understanding how do we make the most of the capacity that we’ve got available to us. So the booking and scheduling processes and the teams behind the scenes that do all the hard work that make sure that we actually have the right patients in the right clinic.
The work involves a lot around 642 meetings, utilisation meetings, getting the data clean so that we really understand what we’re looking at and what we mean when we’re showing utilisation figures and then being able to physically have the right structures within the booking teams to fill that capacity.
So it’s easy to fill six, six weeks out, but actually the difficulty is keeping hold of those patients when cancellations start coming through. So a lot of the work was about how do we backfill those slots that are cancelled at short notice? How do we make sure that we’ve got the capacity within the booking teams to be able to handle the mass that comes through at short notice? and then how do we make sure we’re contacting the right patients to be able to do that?
Just going to have a quick look at what the poll is showing here.

So we’ve got 18 responses and I think, yeah, so, so general consensus, the problem that trusts are facing at the moment is the demand continues to grow and resources are limited. So how do we deal with that lack of capacity in the face of demand?
I think that’s a general theme that comes up when we do these sort of these sort of projects and we do a lot of work around demand capacity modelling, but actually all of these are issues that do crop up in outpatients and it’s interesting we’ve got a 17% split between three of them there, so equal relevance for those three.
As we move through. I think some of these points are likely to be covered off in the conversation. But what I’d like to do is just have some time to to look at the the actual results of the projects.
With Andrina and Sian and just talk to them about how they’ve managed to maintain those results.
OK. So SATH first, so Andrena, we’ve got three graphs here and they’re all showing some pretty stark trend lines. It would be great if you could talk to us a little bit about what the results have looked like for you off the back of the project and what it was that’s really helped you to achieve those benefits.
Andrena Weston (THE SHREWSBURY AND TELFORD HOSPITAL NHS TRUST)
Yeah, absolutely. So as you can see from the first graph, our total waiting list size has reduced and it is still continuing to reduce actually. And I think that is very much supported by the work that we have done with four eyes.
In terms of our 18 week compliance, you can again see a month on month improvement and again, we have no reason to believe that that won’t continue to do so. And more importantly really up to the right hand side is our booked utilisation. So this clinic utilisation and since we implemented or started the project with Four Eyes in April, you can really see that we have really started to improve our booking utilisation and we do think at this point in time we’ve potentially improved by 3-4 percentage points and we have calculated the number of slots that that actually represents and thats potentially 15,000 per year across all specialties.
In terms of the work, do you want me to just carry on in terms of the work and benefits, Sam?
Samantha Sullivan
Yeah, if you’ve if you’ve got any other points to make, go for Andrena.
Andrena Weston (THE SHREWSBURY AND TELFORD HOSPITAL NHS TRUST)
Yeah. So there have been lots of benefits with the work that we have done with, particularly with our own booking team because what we did, we found out that they’re working a little bit chaotically and through the work we’ve done with Four Eyes, we’ve implemented simple things like rotas, you know, one for phones, one for booking, and that’s really provided greater focus really in terms of where they are on a day-to-day basis, so they absolutely understand. So there’s been a real focus there which has improved our booking utilisation. I’ll stop there, Sam. Thanks.
Samantha Sullivan
Can I just ask, so since the project finished in the summer, have there been any fresh challenges that have come up that maybe you weren’t expecting or how has it all worked?
Andrena Weston (THE SHREWSBURY AND TELFORD HOSPITAL NHS TRUST)
Well, we we have had our challenges. I mean the the the things that we did implement when you were working with us back in April and and they’re difficult things to tackle, but they are so worthwhile doing.
So we’ve introduced those specialty booking guidelines and and we did think that you know when we looked at them, when your team looked at them with us in detail, some of them were really, really complex. Some of the booking guidelines were up to 15 pages long, so you’ve really helped condense that and simplify it. And now we’re able to move our teams around and they’re able to pick up that work and and go particularly supporting annual leave or sickness.
The broadcast messaging that you supported us with with Dr Doctor has really, really helped. So now we’re able to fill those last that those last those gaps really within clinics at the last minute and we’re able to fill those and rather than just ringing patients, we’re able to use broadcast messaging. So we are seeing an increase in in utilisation there.
The booking governance group, that was a real game changer for us really because we’ve we it’s enabled us to standardise around even just simple things like how clinics were structured and that has really improved our data quality.
We’ve introduced the 642 meeting for outpatients, which has been a real challenge and we are still getting to grips with that, but that has given us a real clear overview now that the whole of our clinic estate.
In terms of the benefits, I mean they are endless actually, but I think because we have seen that booking utilisation improvement and we’ve been feeding that back regularly to our teams, we have found you know that it really has significantly boosted their morale and consequently absolutely has enhanced their performance.
One of the challenges I would just highlight is because of the use of Dr Doctor now across the majority of our specialties, it’s sort of led to a definitely a reduction in phone calls, which is real positive, but it has increased the workload within the Dr Doctor platform. So there are occasions, where the teams do need to focus on that to obviously, you know, manage those queries, etcetera. But that that’s it for me really. It’s been really positive. Thank you.
Samantha Sullivan
Thanks, Andrina.
Sian, you’ve been at this for two years now. So it’s it’s great to see that actually the results are sustaining there as well. Here’s the graphs for Walsall.
So before we get into this. We’re going to put a word cloud out for everybody on the call. And what we’d like to do is just understand what are the challenges that you face when you’re trying to sustain productivity improvement.
Word cloud (participants enter their challenges):
What makes sustaining a productivity improvement difficult for you?
So I mean we’re talking about outpatients here, but really when it comes to the sustainability part, it’s it’s all the same across all services. So what I’d really like to know, Sian, is what’s what’s it taken from your team to be able to sustain this for two years?
Sian Webley (WALSALL HEALTHCARE NHS TRUST)
Thanks, Sam. So in terms of what it’s taken from the team, we’ve got real strong divisional and executive leadership when it comes to outpatient utilisation and what we’ve really done is try to incorporate it as part of our business as usual.
So the graphs that you see in here today are actually graphs that the team look at at least every week and we report to the executive team every two weeks through our elective care meeting. So we have really incorporated this part of kind of business as usual in terms of commitment from the admin teams who do the booking on a day-to-day basis.
We really tried to give them the autonomy to own this project as their own kind of performance improvement project and empower the teams. It has led to them being extremely proud of some of these metrics that you can see on screen today and they continue to drive performance improvement. So within kind of 6 to 12 months after working with Four Eyes, we were up at our target of 93% booked clinic utilisation and then kind of pushed the team further to say what what more do you think you can do?
And last year we got up to 95% utilisation this year again kind of pushing for 97. But you know that’s working with the teams, but giving them the autonomy and saying actually what do you think you can do and and they do strive to continue to improve that. The DNA rate has been my nemesis a little bit in this trust we started at 11%, got down to 9 with Sam and the Four Eyes team and are now hovering at around 8%. That’s taken some more kind of targeted work with the teams looking at high DNA rate clinics in particular, and we’ve had to do unfortunately some physical phoning of those patients which has really helped. But yeah, in terms of the commitment, it is a senior leadership commitment that this is the right thing to do for our patients and make sure we’re making full use of resources, but also from the teams in kind of owning the quality improvement, performance improvement.
Samantha Sullivan
Thanks, Sian. Can we see the the word clouds?

It’s my first time looking at one of these, so it’s really interesting. The way this works, if you’re not familiar with them, everybody’s written in their responses and then it’ll pop up with the the most common responses. So engagement and conflicting priorities coming through there is some of the key things that is stopping the productivity improvement that you might be seeing from your own projects from sustaining.
Sian, just thinking about those, those sort of challenges that have come through there when people are trying to sustain a productivity improvement, if you could offer some advice to somebody that’s just finished this sort of work, what would it be?
Sian Webley (WALSALL HEALTHCARE NHS TRUST)
I guess both the conflicting priorities and engagement. One for me would be, one – how you’re going to continue to maintain oversight. So I’ve mentioned you know we we have this as part of our business as usual and it really is embedded as business as usual. We have maintained kind of the slot that we had with Four Eyes for a task and finish group, we’ve maintained that slot and kind of developed it as an outpatient transformation group building on the success that we’ve already got.
The other thing that I’d mentioned is just continually reviewing and refreshing what you think your vision is. So I’ve mentioned you know you don’t just finish a project, you say, yeah, we’ve got to the target, we’ve finished the project. Now if we’d have done that with Four Eyes, we’d probably slip back to where we were. But that continual refresh of actually we’re we’re here at 93% now actually what can we do to go further because we all know in terms of conflicting priorities that, actually, this is just bread and butter, basic kind of OPS and us getting the processes right.
The conflicting priorities obviously come from actually when you’re trying to manage a massive PTL that’s out of control and sometimes actually taking it back to the basics will help you to deliver those improvements that you need in your PTL.
One of those old-fashioned phrases, isn’t it? How to eat an elephant a little bit at a time. But I do believe us getting these processes in bookings correct in the first place has has paid dividends on kind of managing and what felt like an unworldy PTL post COVID.
Samantha Sullivan
Andrena, so, so you’re three months in, things have started to bed in. I think I’ve, I’ve seen the teams like people are actually, you know, they’re following the process as it is all working. But like we said, the challenge is really sustaining that long term. So if you could ask somebody that’s been at this for two years one question, what would it be?
Andrena Weston (THE SHREWSBURY AND TELFORD HOSPITAL NHS TRUST)
So I think the main question would be how do we maintain the engagement?
Samantha Sullivan
Sian, what do you think to that?
Sian Webley (WALSALL HEALTHCARE NHS TRUST)
Shall I come into that? So just repeating on some of the other things I’ve said around incorporating it, it’s business as usual. There was a real feel for us in terms of connecting this to the why, and for us at the time that was patients waiting far too long for elective care treatment. So really trying to drive down that wait to first appointment.
I think these graphs that you’re seeing here and being able to re reflect to the teams where they’ve come from. Where they’re going and actually re reflecting those achievements to them and actually this was something to be really proud of and the teams are really proud of it. And then making sure that the teams have the autonomy to go away and drive this themselves, but knowing that we’re here as a senior leadership team to kind of unlock any barriers they’ve got so, you know, I’ve been involved in all sorts of really odd bits from kind of printers not working and causing lots of delays in outpatients to to even more tricky situations. So yeah, really empowering the teams, creating that energy around it as well. You know, I’m really lucky with the team here. They can see how far they’ve come. They can see the impact that we’re having on patients by improving access. And yeah, just getting getting that energy in the team to keep pushing and wanting to change and go further.
Samantha Sullivan
You know, one of the things I remember when we did the Walsall project that I thought was really interesting was the engagement from the patient communication team.
So Gareth [from Walsall Healthcare NHS Trust] got so behind this project, didn’t he? And he became one of the work stream leads, which isn’t the way that we would normally do it, to be honest, like they don’t normally get that involved, but actually I think probably because of his involvement, patients really felt the benefit and your complaints, patient complaints reduced by 14%, so it’s it’s a different type of benefit to the ones we’re showing here, but actually that’s a huge success as well.
Sian Webley (WALSALL HEALTHCARE NHS TRUST)
Yeah, that’s a really good point. So, yeah, when when we think about operational performance, we don’t always include the patient voice in our kind of patient relations teams, do we? But yes, here at Walsall, there’s a really strong patient relations team. And yeah, we brought them into the project and they, yeah, went out and worked with the community. We got feedback, didn’t we? We talked a lot about DNA rates out in the community. So yeah, don’t forget the patient in all this and they can help to kind of design and inform those processes that we’ve got in operational management.
Stephen Dorrell
Samantha, Stephen Dorrell, can I just you asked me at the beginning of this webinar and I didn’t do this, so that’s why I’m interfering now, not forgetting the patient and not forgetting other people on the webinar as well. If you’ve got a comment or if you’ve got a question you want to put to either to Andrena or to Sian, then please do put it in the chat and we will pick it up and try and ensure that the theme that might be burning your mind is is put to the panel so that this can become a discussion around the points of interest to the people who are on the webinar. A point I should have made at the beginning. Apologise for not doing so.
Samantha Sullivan
Thanks, Stephen.
So I suppose what’s interesting is, is what happens next. So you’ve got your foundations in place. You’ve both seen fantastic results and your utilisation is where you want it to be, your waiting lists are starting to come down. But like we said at the start, there’s so much going on in the outpatient space at the moment. This is just the beginning. So it’s really interesting to understand what what’s your next steps in that outpatient transformation. Andrena, do you want to talk about that a little bit?
Andrena Weston (THE SHREWSBURY AND TELFORD HOSPITAL NHS TRUST)
Yes, certainly.
So I think our next steps in terms of the outpatient transformation is to continue our journey with the Dr Doctor roll out. I think the teams have really embraced that, to be honest, it has been a real game changer and it’s something that we have just literally only introduced at the 1st of September, so there is still quite a lot of embedding to do with that.
I think for us as well what we do need to to understand really are our clinic templates and you know looking reviewing those and and yourselves and the team are with us at the moment to support us with that. But I think you know outpatients is, you know, all patients are seen in outpatients. So it is really, really important that we absolutely maximise our throughput and working with our team, particularly within the booking team is a centralised team. They absolutely do need to be supported.
And I think what we do need to do is to make sure that they have the tools available, digital tools available to do their jobs more effectively really.
And as Sian said, you know, our COO [Chief Operating Officer, Ned Hobbs] was previously the COO at Walsall and is very, very engaged with this process along with the deputy COO [James Wright]. So there is real support with us now we we feel like we’re doing it as a trust now and also that that patient buy in as well I think is is particularly important. But next steps really is really looking at our clinic templates and the timings of our appointments, which is a big piece of work, so thank you.
Samantha Sullivan
Certainly is. What about you, Sian? What’s going on at Walsall now?
Sian Webley (WALSALL HEALTHCARE NHS TRUST)
So for us last year we started referral assessment in some of our subspecialties. So reviewing those referrals before we kind of accept them if you like, looking at what we could kind of divert to advice and guidance. So didn’t need to come straight into a face to face appointment.
What I’m really keen to do now is obviously we’ve we’ve got the utilisation of our clinics now we’re filling the clinics, we’re still driving down the DNA rate. What I’m really interested in is are we seeing the right patients in clinics, so what I want to look at is actually what percentage of patients are coming to clinics and then going on to a diagnostic and actually whether we can flip that around to make sure that our appointments are value added.
Because you know everyone takes time off to go to a hospital appointment, you can sit for a delayed period unfortunately waiting in outpatients just to then be told that you need a diagnostic, and you know, I think that will help us again continue to drive down the PTL in terms of making sure that we’re adding value when the patient gets to see a consultant, it’s not just a you need a scan, go away and come back again. Actually just making sure that those are really value added and that we can maximise making sure that patients either have a decision to treat or are treated at their first appointment.
Stephen Dorrell
Just to draw out Sam, the the the question from Debbie in the chat was ‘were the outpatients department nursing team involved?’ and Sian has given a very emphatic yes to that and I’m sure Andrena would answer give the same answer as well.
Andrina the engagement of the nursing team.
Andrena Weston (THE SHREWSBURY AND TELFORD HOSPITAL NHS TRUST)
Yeah, absolutely. I was just typing it in the chat.
But yes, our our outpatient nurses are heavily involved and and particularly through our 642 process that that we have introduced and I think that is helping them, their engagement is really helping them support their staffing allocation and things like that. So yes, that they’re they’re pivotal, absolutely pivotal.
Samantha Sullivan
I think some of the the key messages coming through here is all about engagement really, isn’t it? So it’s that get get your foundations right before you move on to some of the more innovative stuff and that helps you to gain the confidence of of the clinical team and the Ops team. But I think engagement throughout is really key to make this a success and to make it sustain.
We’ve just got a couple of minutes left. I don’t know if there’s any other questions that people have got.
Stephen Dorrell
Tap away in the it gives a an opportunity. We’ve got a couple of minutes left and if there’s a question that appears in the chat, we’ll pick it up. But I’ll use the moment, if I may, just to say thank you first of all for attending the webinar. I would hope you found it instructive and helpful. And there will be a recording of the webinar that be sent via e-mail to everyone who’s attended and indeed we will forward it to anyone else who might be interested as well.
So, do you have a concluding comment, Sam?
Samantha Sullivan
Yes. So I suppose just to say thank you all again for for coming along today.
Outpatients is something I’m passionate about and I’m really pleased that it’s come to the forefront and suddenly it’s, you know, it’s hot topic. So it’s it’s nice to see that everyone is kind of rallying around trying to make our patients as successful as they can and starting to look at all this stuff in a bit more detail. So thank you all for coming today and that’s that’s it from me.
Stephen Dorrell
OK. And a huge thank you to Sian and to Andrina for sharing their experience with us and for saying for for demonstrating actually on the graphs you put on the screen. Thank you, the effectiveness of how you can make a difference.
These things are not cast in stone. It is possible to do it differently and to respond, even if that doesn’t constitute what Jim Mackie might call tearing up the outpatients model. It definitely involves doing it different and doing it better from everybody’s point of view.
So thank you to Andrina, thank you to Sian and thank you to Sam for organising it and most importantly, thank you to everyone for for joining. Good afternoon. We finished more or less on time. Thank you.
Ends.
Contact us to learn how we can support your outpatient improvement.