Case Study
Go Back-
Case Study > Case Study: How SaTH is Creating Thousands of Additional Appointments
Case Study: How SaTH is Creating Thousands of Additional Appointments
Unlocking Hidden Capacity: How SaTH is Creating Thousands of Additional Appointments with clinic template optimisation
A Four Eyes Insight and Prism Improvement Programme
Across the NHS, waiting lists remain a persistent challenge. But what if the solution isn’t always about more funding or more staff? What if significant capacity is already there, waiting to be unlocked?
At Shrewsbury & Telford NHS Trust, a 20-week Clinic Template Optimisation Programme has proved that smart analysis and clinical collaboration can deliver remarkable results.
The Challenge
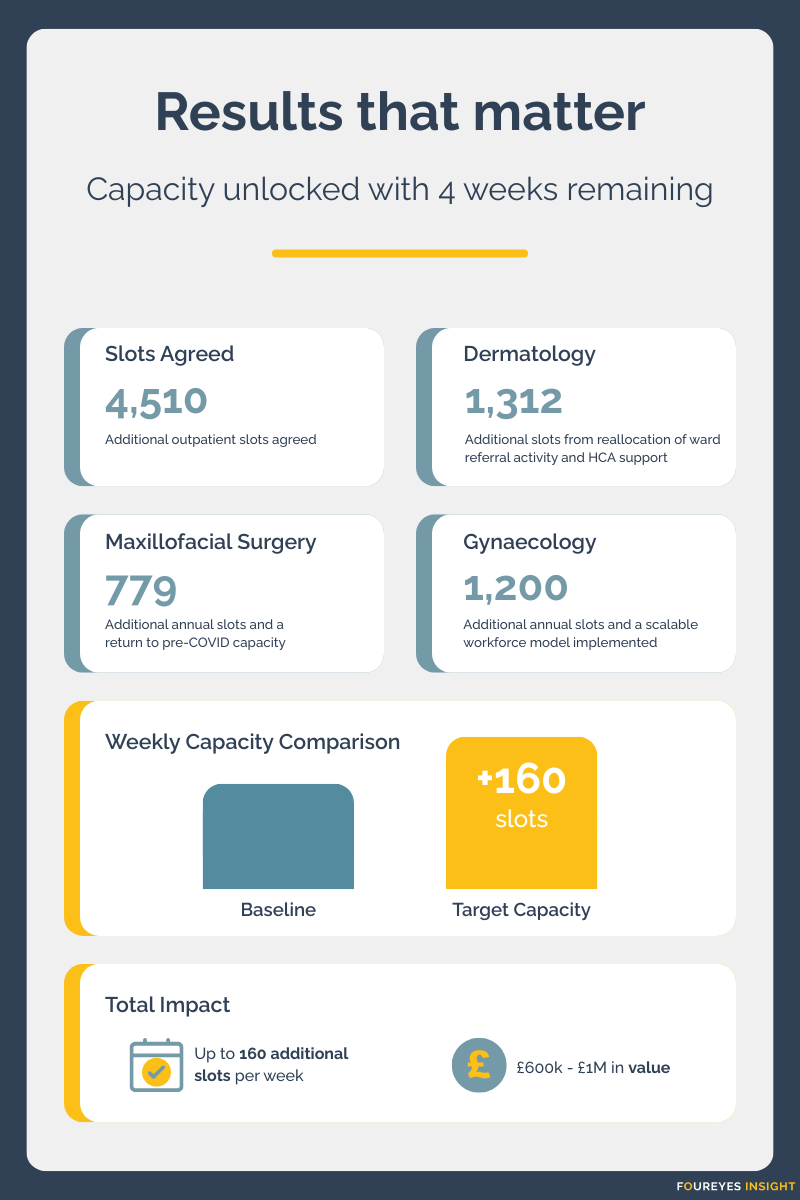
Like many trusts, Shrewsbury & Telford needed to increase clinic capacity and create additional appointment slots. The goal was ambitious: release up to 160 slots per week across 8 core specialities, representing between £600,000 and £1 million in value.
A Systematic Approach
Rather than implementing top-down changes, the programme took a methodical, collaborative approach built on four key steps.
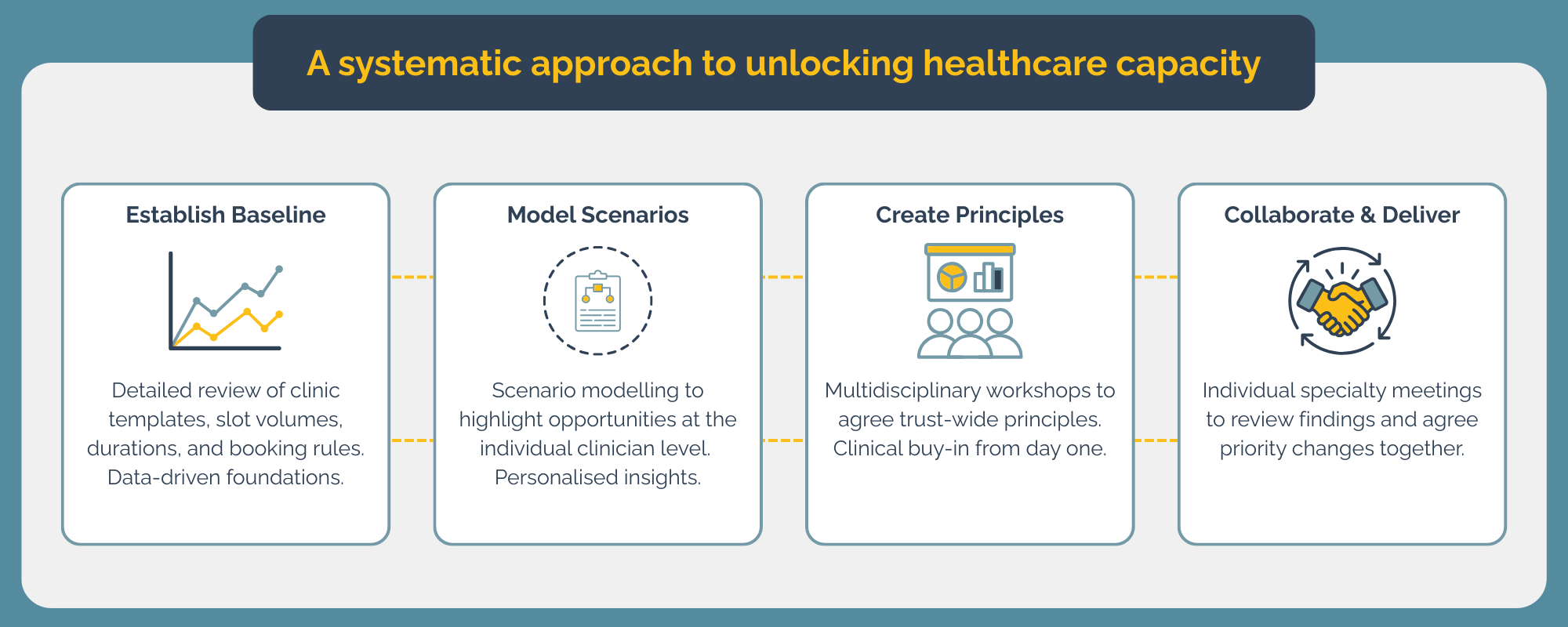
First came establishing a clear baseline. The team conducted a detailed review of clinic templates to understand who delivers each element of activity, identify multi-codes within sessions, and capture essential structure including start and finish times, slot volumes, durations, and booking rules. No assumptions, just data.
With the baseline set, scenario modelling highlighted the strongest opportunities at individual clinician level. This personalised approach ensured that recommendations were practical and reflected the reality of how each clinician works.
The insights were then brought into multidisciplinary workshops to agree trust-wide principles that each clinic should follow. This created clinical buy-in from the start, ensuring that changes would be both clinically safe and operationally sustainable.
Finally, individual meetings with each specialty allowed teams to review findings together and agree on priority changes. This collaborative approach transformed what could have been a contentious process into a genuine partnership.
Results that matter
Through the Clinic Template Optimisation Programme, 4,510 additional outpatient slots have been agreed across participating specialties, achieved not through additional funding or estate expansion, but by better aligning workforce capacity to clinical demand.
Crucially, many of these gains are being delivered by reconfiguring how existing staff are deployed, rather than increasing headcount.
In Colorectal, one additional new patient clinic per week has been agreed for registrars, delivering six new patient slots per clinic. This has been enabled by reallocating mid-grade staff from ward-based activity into clinics, directly increasing outpatient capacity while maintaining clinical oversight. This equates to an annual increase of approximately 252 additional slots.
In Gynaecology, four new clinics have been established alongside the introduction of a new mid-grade rota launched in December 2025. This includes Registrar and SHO-led clinics, each delivering seven patient slots, with scope to increase capacity further once the rota is fully embedded. This change improves predictability of workforce deployment and supports sustainable clinic delivery without increasing consultant workload, delivering an annual increase of approximately 1200 additional slots.
In Dermatology, multiple workforce-enabled changes have been agreed. First, three new clinics will be established, each delivering two new and four follow-up appointments, subject to approval of a business case to appoint one Senior House Officer or Specialist Registrar to take over ward referral activity. This change represents an annual increase of approximately 756 slots, with potential to scale further once embedded.
Second, within four nurse-led clinics, templates will be revised from four universal slots to two new and three follow-up slots, enabled through business case approval to secure chaperone support for paediatric nurse-led clinics. This change delivers an additional 84 slots annually.
Finally, to improve clinic flow, all clinics running under three hours will have one additional slot added, and clinics over three hours will have two additional slots added, subject to approval to employ Health Care Assistants to support clinic flow within the department. Notably, this role could potentially be filled through reallocation of an existing HCA from another department, rather than recruiting additional staff. This change is expected to deliver an annual increase of approximately 388 slots, with impact to be reviewed after three months and scope to increase capacity further depending on clinic flow and performance.
In Maxillofacial Surgery, Minor Operations clinics have returned to pre-COVID capacity, increasing from six to seven slots per clinic and delivering an additional 210 appointments annually. Further progress has been driven through clinical-lead-led standard setting aligned to GIRFT upper-quartile benchmarks.
The Clinical Lead has agreed template changes within their own clinics, redesigning general clinics from nine universal slots to a clinically optimised mix of five new and six follow-up appointments, alongside the addition of one further follow-up slot in skin clinics. Together, these changes deliver an additional 97 appointments per year.
While these standards have currently been agreed by the Clinical Lead only, they establish a clear benchmark for the specialty. Early adoption by other consultants is already emerging, for example Tun Wildan’s agreement to add additional capacity across oncology, skin and general clinics, indicating further capacity gains as these standards are embedded more widely.
The Key Lesson
The real insight from this programme isn’t just about the numbers, impressive though they are. It’s about the approach. Sustainable capacity gains in healthcare come from combining rigorous data analysis with genuine clinical collaboration.
When frontline teams are brought into the solution rather than having changes imposed upon them, transformation becomes not just possible but sustainable. The data reveals the opportunities, but it’s the clinical expertise that determines which changes will actually work in practice.
For other trusts facing similar capacity challenges, the message is clear: before looking externally for solutions, look internally at how current capacity is being used. The appointments patients need might already be there, just waiting to be unlocked.
About
The Clinic Template Optimisation Programme at Shrewsbury & Telford NHS Trust demonstrates how operational excellence and clinical collaboration can deliver significant capacity gains without additional resources. Contact us to learn more about how Four Eyes Insight can support you.